Article Text
Abstract
Fasting the Holy month of Ramadan constitutes one of the five pillars of the Muslim faith. Although there is some evidence that intermittent fasting during Ramadan may be of benefit in losing weight and cardiometabolic risk factors, there is no strong evidence these benefits apply to people with diabetes. The American Diabetes Association/European Association for the Study of Diabetes consensus recommendations emphasize the importance of patient factors and comorbidities when choosing diabetes medications including the presence of comorbidities, atherosclerotic cardiovascular disease, heart failure, chronic kidney disease, hypoglycemia risk, weight issues and costs. Structured education and pre-Ramadan counseing are key components to successful management of patients with diabetes. These should cover important aspects like glycemic targets, self-monitoring of blood glucose, diet, physical activity including Taraweeh prayers, medication and dose adjustment, side effects and when to break the fast. The decision cycle adapted for the specific situation of Ramadan provides an aid for such an assessment. Children with type 1 diabetes should strongly be advised not to fast due to the high risk of acute complications such as hypoglycemia and probably diabetic ketoacidosis (DKA), although there is very little evidence that DKA is increased in Ramadan. Pregnant women with diabetes or gestational diabetes should be advised to avoid fasting because of possible negative maternal and fetal outcomes. Hypoglycemia is a common concern during Ramadan fasting. To prevent hypoglycemic and hyperglycemic events, we recommend the adoption of diabetes self-management education and support principles. The use of the emerging technology and continuous glucose monitoring during Ramadan could help to recognize hypoglycemic and hyperglycemic complications related to omission and/or medication adjustment during fasting; however, the cost represents a significant barrier.
- endocrinology diabetes
- gestational diabetes mellitus
- nutrition
This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, remix, adapt, build upon this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited, appropriate credit is given, any changes made indicated, and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0/.
Statistics from Altmetric.com
INTRODUCTION
Fasting the Holy month of Ramadan may be challenging for the people with diabetes and their care providers due to potentially increased risk of acute complications such as hypoglycemia, hyperglycemia, dehydration and probably diabetic ketoacidosis (DKA), although there is very little evidence that DKA is increased during Ramadan.1 Hence, in 2005, the first statement for management of diabetes during Ramadan was published as an American Diabetes Association (ADA) working group report2; after receiving multiple inquires asking for regular updates addressing the most important issues not covered in the initial document, the authors decided to do regular 5 yearly updates.3 4 In this 2020 update, we aimed to apply the principles of ADA/European Association for the Study of Diabetes (EASD) type 2 diabetes management guidelines to Ramadan. New sections on the management of children with type 1 diabetes and pregnancy are included. We have carefully reviewed the literature and published data on medical nutrition therapy (MNT) and the use of glucose-lowering medications during Ramadan.2
It is estimated that the total Muslim population worldwide approached 1.9 billion as of 2019, which includes about 24.4% of the world population.5 Based on the recent International Diabetes Federation Atlas Ninth Edition 2019 report on the prevalence of diabetes of 463 million or 9.1% worldwide,6 one can estimate that almost 112 million people with diabetes worldwide may choose to fast during Ramadan.
Fasting the Holy month of Ramadan constitutes one of the five pillars of the Muslim faith, it is obligatory for all adult Muslims. Although, illness constitutes exemption from fasting,7 a vast majority of Muslims with diabetes do not consider themselves unwell and exempted and choose to fast. This should be respected, and such patients should be supported to help them fast.
Ramadan fasting may have a positive effect on increased self-esteem, promoted psychological stress, decreased anxiety and stress, self-control and the ability to sympathize with others,8 however very few studies have looked at the emotional consequences of short-term Ramadan fasting in healthy people versus people with diabetes, this could be an interesting future research point where the directional hypothesis needs to focus on mood changes, irritability, feeling of reward, fear of punishment and self-restrain and control and sexual behavior will be few interesting avenues with larger and diverse sample size via a robust statistical testing.
INTERMITTENT FASTING
Intermittent fasting is an eating pattern where you cycle between periods of eating and fasting and is increasing in popularity as a mean of losing weight and controlling chronic illness.9 It could be for religious reasons or non-religious reasons like losing weight. The Ramadan fast is a form of intermittent fasting where the normal eating pattern shifts to exclusive nocturnal eating. Based on the current available evidence and knowledge, intermittent fasting can be safe in people with diabetes when done under medical supervision and may reduce body weight, central adiposity and glycated hemoglobin (HbA1c). There is also evidence that intermittent fasting improves insulin sensitivity and cardiovascular disease (CVD) markers.10 It should be noted that unlike most forms of intermittent fasting, Ramadan fasting involves no intake of water/fluids. Also, intermittent fasting has the potential for hypoglycemia in patients receiving antidiabetic medications associated with hypoglycemia such as sulfonylureas (SU) and insulin therapy.11
APPLYING THE PRINCIPLES OF THE ADA/EASD CONSENSUS
The ADA/EASD consensus report 2018 and its recent update provides comprehensive recommendations on the management of hyperglycemia in patients with type 2 diabetes incorporating the evidence from the outcomes of new trials into decision making.12–14 The report considers major aspects of type 2 diabetes management including the presence of comorbidities such as atherosclerotic cardiovascular disease (ASCVD), heart failure (HF), chronic kidney disease (CKD), hypoglycemia risk and weight management. It gives recognition to patient-centred care, optimization of quality of life and reducing burden of complications. This consensus recommendation applies to most scenarios encountered in the Holy Month of Ramadan observed by Muslim patients with type 2 diabetes. The ADA/EASD consensus does not address the management of type 1 diabetes for which relevant guidance is available.4 15
Applying the principles of decision cycle in the management of patients with type 2 diabetes who observe Ramadan fasting
The key to successful diabetes management in Ramadan should be no different and the general aim is control of symptoms, prevent deterioration in glycemic control and prevention of acute complications.
The decision cycle for patient-centred glycemic management in type 2 diabetes provides an aid for healthcare professionals (HCPs) while proposing and making management decisions for Muslim patients with type 2 diabetes who are planning to fast during Ramadan (figure 1). This has been adopted and modified specifically for Ramadan based on the ADA/EASD consensus recommendations 2018.
Decision cycle for patient-centred glycemic management in Muslim patients during Ramadan. Modified and adopted from Davies et al.13 ASCVD, atherosclerotic cardiovascular disease; BD, twice a day; CKD, chronic kidney disease; DKA, diabetic ketoacidosis; HF, heart failure; HHS, hyperosmolar hyperglycemic state; MNT, medical nutrition therapy; OD, once a day; SMBG, self-monitoring of blood glucose.
Pre-Ramadan assessment including assessment of key patient characteristics, treatment choice and shared decision making
Pre-Ramadan counseling and clinical assessment is essential component of managing patients with type 2 diabetes during Ramadan. This should comprise assessment of areas highlighted in decision cycle, including key patient characteristics like age, frailty, lifestyle, cultural and socioeconomic factors and presence of comorbidities with risk stratification as highlighted in box 1.3 4
Categories of risk in patients with type 2 diabetes who fast during Ramadan
Very high risk: fasting not recommended
Severe hypoglycemia within the 3 months prior to Ramadan.
Severe hyperglycemia with average fasting or premeal plasma glucose >16.7 mmol/L (300 mg/dL) or glycated hemoglobin (HbA1c) >86 mmol/mol (10%).
A history of recurrent hypoglycemia or hypoglycemia unawareness.
Diabetic ketoacidosis/hyperosmolar hyperglycemic state within the 3 months prior to Ramadan.
Acute illness.
Performing intense physical labor.
Pregnancy.
Chronic dialysis.
Patients with significant dementia or cognitive deficits.
High risk: may choose not to fast
Moderate hyperglycemia (average blood glucose 8.3–16.7 mmol/L (150–300 mg/dL) or HbA1c 64–86 mmol/mol (8%–10%)).
Significant microvascular or macrovascular complications.
Living alone and treated with insulin or sulfonylureas.
Patients with comorbid conditions that present additional risk factors like heart failure, stroke, malignancy, renal impairment.
Elderly >75 years of age.
Moderate risk: may choose to fast with caution
People with type 2 diabetes with no complications and HbA1c <64 mmol/mol (8%) treated with lifestyle intervention, metformin, thiazolidinedione (TZD), incretin-based therapies, sodium-glucose cotransporter-2 inhibitors* and/or short-acting insulin secretagogues.
Low risk: may choose to fast
People with type 2 diabetes with no complications and HbA1c <53 mmol/mol (7%) treated with lifestyle intervention, metformin, TZD and/or incretin-based therapies.
Diabetes management plan during Ramadan
Review management plan and adjusting treatment regimen is required during Ramadan to avoid hypoglycemic and hyperglycemic events. Suboptimal adherence to medication, fear of hypoglycemia, medication adverse effects and lack of access to medication should be identified and addressed prior to Ramadan fasting.
It is important to inform patients that blood glucose testing during Ramadan does not break the fast; a common misconception in some parts of the world. Blood glucose should be regularly monitored during fasting, especially those on insulin or insulin secretagogues.
All patients should be educated about the symptoms of hypoglycemia, and to stop the fast in case of symptoms of hypoglycemia, hyperglycemia, dehydration or acute illness occur and blood glucose level of <3.9 mmol/L (<70 mg/dL) or >16.6 mmol/L (>300 mg/dL).16
Use of self-monitoring of blood glucose (SMBG) should be individualized during Ramadan with need for more frequent monitoring in those at higher risk of hypoglycemia, especially in regions with longer fasting hours or warmer climate.
The use of novel technologies such as continuous glucose monitoring (CGM) is currently not routinely recommended for patients with type 2 diabetes.17
Structured education for patients planning fasting
The role of a structured education in patients with type 2 diabetes is well established,18–25 and this benefit is also proven in Muslims with diabetes practicing Ramadan.26–32 In a retrospective study, patients receiving pre-Ramadan education experienced less hypoglycemia.26 It is important that the structured education is implemented and ideally it should incorporate community awareness package, HCP training and patient self-management course like ‘A Safer Ramadan’.33
The therapeutic options for fasting patients with type 2 diabetes during Ramadan including lifestyle, weight management and medications
Lifestyle management
Medical nutrition therapy and dietary patterns for Ramadan
Medical nutrition therapy should be provided by a registered dietitian or nutrition professional34 and should include principles of healthy eating behaviors, preventive methods for hypoglycemia, proper portion intake.35 Since foods consumed during Ramadan tend to be higher in carbohydrate, strategies should include portion control as well as the possible incorporation of physical activity after meal. The DAR International Alliance has developed the Ramadan Nutrition Plan, a web-based tool designed to help HCPs in delivering patient-specific nutrition education for Ramadan.36
A frequently ignored aspect is food consumption during Eid, which is the 3-day festival after Ramadan involving high consumptions of calories and carbohydrates with family and friends.
Dates consumption
Daily consumption of dates is a deeply rooted tradition among Muslims, especially during Ramadan. The habitual eating patterns have changed recently; however, consumption of dates remains in most countries. The highest consumption of dates was found among Arab Gulf populations,37–40 with a daily date intake in these countries between 68 and 164 g.40 It is actually recommended to break the fast on dates, as Prophet Mohammad (peace and blessings be on him) used to do. Dates have a low glycemic index (GI) provided it is consumed in a small amount. Therefore, up to two to three dates can be eaten safely when breaking fast.41
Physical activity and Taraweeh prayers
Although increased physical activity should generally be encouraged in all patients with type 2 diabetes, but during Ramadan it warrants caution. The Taraweeh prayer during Ramadan after Iftaar meal involves repeated cycles of rising, kneeling and bowing and should be considered as part of daily exercise.4 Physical activity should be encouraged for people with diabetes and normal levels may be maintained during the month of Ramadan. However, excessive physical activity may lead to a higher risk of hypoglycemia and should be avoided, especially before the sunset meal, in those with high risk of hypoglycemia and those on insulin or insulin secretagogues.3
Glucose-lowering medications
Summary of the recent ADA/EASD update 2019 to the ADA/EASD consensus 2018
It is recommended that decision to start a new glucose-lowering medication should be made in advance of start of Ramadan and dose adjustments or medication reviews are done accordingly, especially if hypoglycemia or tolerability becomes a concern during fasting. The ADA/EASD 2018 consensus12 13 and its recent update14 recognize presence or absence of ASCVD, HF and CKD an important early step in treatment selection (figure 2). This is based on the outcomes of various Cardiovascular Outcome Trials mainly involving glucagon-like peptide-1 receptor agonists (GLP-1RA) and sodium-glucose cotransporter-2 inhibitors (SGLT2i).42–52
Glucose-lowering medications use before and during Ramadan. Modified and adopted from Davies et al.13 *For intensification beyond dual therapy, choose option with lower risk of hypoglycemia. **Consider sulfonylurea (SU) or basal insulin with lower risk of hypoglycemia. ASCVD, atherosclerotic cardiovascular disease; CKD, chronic kidney disease; DKA, diabetic ketoacidosis; DPP4, dipeptidyl peptidase-4; GLP-1RA, glucagon-like peptide-1 receptor agonists; HbA1c, glycated hemoglobin; HF, heart failure; HHS, hyperosmolar hyperglycemic state; SGLT2i, sodium-glucose cotransporter-2 inhibitors; SMBG, self-monitoring of blood glucose; TZD, thiazolidinedione.
A key new recommendation in the ADA/EASD consensus update is initial combination therapy including metformin in newly diagnosed patients with type 2 diabetes based on the outcome of VERIFY (Vildagliptin Efficacy in combination with metfoRmIn For earlY treatment of type 2 diabetes) trial.53
Glucose-lowering medications and Ramadan
Metformin: Metformin has a long history of safety and efficacy and remains the first-line medication for management of type 2 diabetes12 13 either alone or in combination.14 Usually, no dose change is advised during Ramadan, but timings need to be reviewed for Ramadan.
Sodium-glucose cotransporter-2 inhibitor (SGLT2i): Since the last Ramadan update in 2015,4 several studies have shown the safety of the SGLT2i class during Ramadan including lower risk of hypoglycemia and renal safety.54–57 However, careful pre-Ramadan assessment and education is important including advice on hydration and potential risk of volume contraction and postural hypotension, especially in warm climates with long fasting hours and risk of diabetic ketoacidosis (DKA). Testing for ketones when unwell is required for all patients who chose to fast and are using SGLT2i.15 Patients should be encouraged to drink extra fluids during permissible hours and should have clear instructions when to break fasting, especially if vomiting or positive ketones even with normal blood glucose levels. We generally recommend not starting SGLT2i as a new medication during or immediately prior to Ramadan and patients should be well established on these drugs prior to start of Ramadan. Elderly patients, those with renal impairment, hypotensive patients or those on diuretics if they are planning to fast for Ramadan, should proceed with caution and consider stopping16 or reducing the dose of SGLT2i.
Glucagon-like peptide-1 receptor agonist (GLP-1RA): GLP-1RA agents are effective in improving glycemic control with low risk of hypoglycemia or weight gain (figure 2). GLP-1RA constitute a very desirable option for fasting patients with weight concerns, high-risk factors for ASCVD or established ASCVD. Randomized controlled trial has reported on the efficacy and safety of treatment with liraglutide in combination with metformin compared with SU during Ramadan.58 Two further studies have also demonstrated the safety and efficacy of liraglutide during Ramadan.59 60 Depending on the formulation used, the GLP-1RA may need to be injected daily or once-weekly. Weekly preparations are an attractive option for fasting patients who prefer a simplified regimen. The most common adverse events of GLP-1RA are GI effects including nausea and vomiting, increasing the risk of dehydration. Thus, it is recommended that GLP-1RA should be started at least 4–8 weeks prior to fasting with titration to tolerated dose before the start of Ramadan.
Dipeptidyl peptidase-4 inhibitor (DPP4 inhibitors): the ADA/EASD consensus recommends DPP4 inhibitors as an add-on option to metformin where there is a compelling need to minimize hypoglycemia (figure 2). DPP4 inhibitors are weight neutral and have a low risk of hypoglycemia but when combined with SU, the risk of hypoglycemia is increased by 50%.61 Generally, no change in the dose of DPP4 inhibitor is required either as monotherapy or combination therapy during Ramadan. Several trials have reported similar efficacy but significant reduction in hypoglycemic events with the use of DPP4 inhibitors compared with SU treatment during Ramadan in patients with type 2 diabetes.62–64
Thiazolidinediones (TZD): TZD use is not associated with hypoglycemia and is recommended as one of the add-on options to metformin in fasting patients during Ramadan, especially when hypoglycemia is a major risk (figure 2). Additionally, TZD is an attractive option in lower middle-income countries where cost consideration is a major issue. TZD should be avoided in patients with history of HF.
Sulfonylurea (SU): SUs have widespread availability but are known to increase the risk of hypoglycemia, which is of great concern during Ramadan. The newer generation SU like glipizide, glimepiride and gliclazide have a lower risk of hypoglycemia compared with older and longer-acting agents.65 This has also been shown in patients observing fasting during Ramadan.66 The Cardiovascular Outcome Study of Linagliptin vs Glimepiride in Type 2 Diabetes (CAROLINA) trial which compared linagliptin and glimepiride, reported similar cardiovascular safety profile, but higher risk of hypoglycemia in glimepiride-treated patients.67 We recommend either substituting or stopping or reducing the dose of SU in patients at high risk of hypoglycemia.
Table 1 gives a summary of recommendations in terms of dose adjustment during Ramadan for non-insulin glucose-lowering therapies.
Recommended medical therapy changes during Ramadan for patients with type 2 diabetes
Other glucose-lowering agents: The meglitinides like repaglinide are shorter-acting insulin secretagogues with lower risk of hypoglycemia compared with SUs but require twice-daily or thrice-daily doses with main meals. One study showed no difference in the incidence of hypoglycemia between groups taking repaglinide and glimepiride.68 Alpha-glucosidase inhibitors are useful for patients with type 2 diabetes who have a tendency for hypoglycemia and therefore a very suitable option during Ramadan.69 The rest of the oral glucose-lowering options like colesevelam, bromocriptine and pramlintide are not discussed due to lack of major new scientific information on these medications and the fact that they are not widely available during Ramadan.
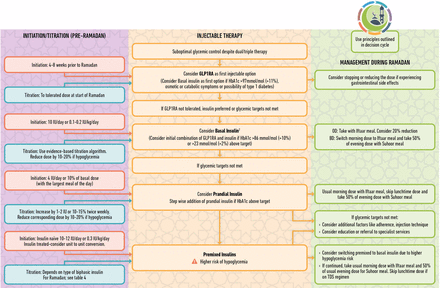
Managing injectable therapies including insulin during Ramadan (figure 3): The ADA/EASD 2018 consensus12 13 recommends use of GLP-1RA prior to insulin as a first-line injectable therapy if HbA1c is above target despite dual or triple oral therapy. In addition, the consensus recommends initial combination of GLP-1RA plus insulin if HbA1c >86 mmol/mol (10%) and/or >23 mmol/mol (2%) above target. The efficacy and safety of insulin is dependent on its appropriate use during Ramadan including patient training and education, diet and activity, dose titration, timing (Suhoor and Iftaar) and type of insulin used. It is very important that patients requiring injectable therapy (either GLP-1RA or insulin) are well established on stable injectable therapy preferably for at least 4 weeks prior to start of Ramadan.
Basal insulin: Basal insulin is the preferred initial insulin regimen in patients with type 2 diabetes (figure 3). Providers should consider insulin preparations associated with less risk of hypoglycemia and to adjust the established dose during Ramadan. In a study comparing use of insulin degludec and glargine in patient with type 2 diabetes, prespecified adjudicated severe hypoglycemia occurred in 4.9% patients in the degludec group and in 6.6% patients in the glargine group, for an absolute difference of 1.7% over 2 years.70 A concern with insulin use, especially in those who require large doses of insulin, is weight gain. In such situations, GLP-1RA therapy combined with basal insulin may result in improved weight, HbA1c and lower risk of hypoglycemia.71–74 Such a combination therapy, however, should be planned well in advance of Ramadan and patients should be on stable doses of insulin and GLP-1RA before the start of Ramadan. Similarly, studies combining SGLT2i and insulin have shown to be a safe and efficient combination in non-fasting patients with type 2 diabetes.75–77 However, the use of insulin in combination with SGLT2i may increase the risk of hypoglycemia during fasting.56 In addition, we recommend reducing the dose or preferably stopping SU therapy when commencing insulin therapy for patients planning to fast during Ramadan.
Other insulin formulations including short-acting insulins and premixed insulins: based on ADA/EASD consensus, we recommend when blood glucose is not adequately controlled with basal insulin, to start short-acting insulins with the two main meals (Iftaar and Suhoor) during Ramadan15 (figure 3). Various premixed insulin combinations are commercially available. Al-Arouj et al recommend switching premixed or intermediate-acting insulin twice daily to long-acting or intermediate-acting insulin in the evening and rapid-acting insulin with meals; with usual dose at Iftaar meal and half usual dose at Suhoor.3 Premixed insulins remain frequently prescribed option in many Muslim countries because of cost and availability issues and if required we recommend usual dose for Iftaar meal and 50% of the usual dose for Suhoor if on twice-daily regimen.
Managing injectable therapy before and during Ramadan. Modified and adopted from Davies et al.13 Consider basal insulin with lower risk of hypoglycemia (degludec/glargine 300<glargine 100/detemir<NPH). BD, twice a day; GLP-1RA, glucagon-like peptide-1 receptor agonists; HbA1c, glycated hemoglobin; NPH, Neutral Protamine Hagedorn; OD, once a day; TDS, three times a day.
Table 2 gives a summary of the recommended changes to different insulin regimens for Ramadan.
Recommended changes for insulin therapy for patients with type 2 diabetes during Ramadan
Hassanein et al78 advocate dose adjustment to premixed insulin dose depending on the blood glucose and we recommend following algorithm for self-titration of premixed insulin during Ramadan (table 3).
Algorithm for premixed insulin titration during Ramadan
Generally, it is recommended to consider stopping or reducing the dose of any glucose-lowering medication with risk of hypoglycemia for Ramadan, particularly if the HbA1c is <48 mmol/mol (6.5%) or if there is a recent history of hypoglycemia.
HYPOGLYCEMIA
Hypoglycemia is by far the most common concern for people with diabetes observing Ramadan fasting, as described previously. The Epidemiology of Diabetes and Ramadan (EPIDIAR) study showed significant increase in all forms of hypoglycemia among people with diabetes during Ramadan fasting.79 Diabetes self-management education and support (DSMES) for prevention and treatment could serve as a good tool to minimize the hypoglycemic episodes during Ramadan fasting. The US National Standards are designed to define quality DSMES and assist those who provide DSMES services to implement evidence-based DSMES.80
EMERGING TECHNOLOGY USE IN DIABETES
There is an increasing recognition of use of technology in diabetes. Blood glucose monitoring, exercise time, medication dosages and energy ingestion can all be digitalized and accessed remotely. Pattern recognition in software is also available to help clinicians make complex decisions. Remote technologies like texts, emails and video-links can improve communication. All this can be used where available to improve care and support for people with diabetes who are fasting during Ramadan. The use of CGM has illustrated the wide variability in glucose levels during fasting and feast.81 82 This information can be a valuable tool, whether used intermittently or continuously, to aid in adjusting medications as well as composition of meals for optimal blood glucose control.83 84
A clinical observational study in Ajman (UAE) examined glucose variability using CGM during Ramadan fasting in patients with type 2 diabetes without insulin treatment.81 They found that patients on SU and on more than two glucose-lowering medications showed early significant increase in mean amplitude of glycemic excursions. They concluded that except for an initial increase in glucose variability, fasting during Ramadan for patients with non-insulin-treated type 2 diabetes did not cause any significant changes in metabolic control, glucose fluctuation or time in hypoglycemia during CGM recording days compared with the non-fasting pre-Ramadan period and pre-Ramadan and early Ramadan patient education and follow-up of high-risk patients may help avoid initial significant glucose variability in patients with non-insulin-treated type 2 diabetes.81
CHILDREN WITH TYPE 1 DIABETES
Management of children and adolescents with type 1 diabetes during Ramadan is highly variable in Arab countries85 and hypoglycemia during daytime fasting remains a major concern. Although the use of CGM may reduce risk of hypoglycemia during Ramadan,86 the fear of hypoglycemia persists. A recent retrospective analysis of children and adolescents with type 1 diabetes during ~3 weeks of fasting showed that approximately 54% of them were on multiple daily insulin injections (MDI) and 46% on insulin pump therapy.87 Although there were no differences between the two groups in breaking days of fasting, patients with HbA1c ≥69 mmol/mol (8.5%) experienced more frequent hypoglycemic attacks than patients with HbA1c <69 mmol/mol (8.5 %). A more extensive meta-analysis of observational studies of young adults with type 1 diabetes revealed similar findings.88 However, despite a lower level of HbA1c before fasting, the insulin pump group had lower rates of severe hypoglycemia than patients treated with MDI.
Defects in epinephrine responsiveness to hypoglycemia have been demonstrated in children and adolescents with type 1 diabetes,89 90 and defects in cortisol particularly at night have also been seen.91 Children with type 1 diabetes should strongly be advised not to fast. Children and adolescents with type 1 diabetes and their families need careful education and management of their insulin regimen and CGM to reduce the risk of hypoglycemia during Ramadan,87 if planning to fast.
PREGNANT WOMEN WITH DIABETES OR GESTATIONAL DIABETES
Most guidelines have advised against fasting for pregnant women with diabetes during Ramadan.4 16 Despite the clear religious and clinical guidance, alarming reports of 59%–90% show that pregnant and lactating Muslim women fast during Ramadan.92 93
Maternal outcomes
Research looking into the effect of maternal diet restriction during Ramadan fast on maternal and perinatal outcomes and/or metabolic changes has resulted in conflicting and insufficient result.94
A small study in rural West Africa in lactating and pregnant women with diabetes showed metabolic derangements in late pregnancy that were suspected to be due to accelerated starvation that may occur in late pregnancy.92 Similar metabolic derangements in those with and without diabetes during pregnancy were reported by other authors.95 96 A study in Emirati pregnant women without diabetes found a significantly higher 1 hour postprandial glycemia in pregnant women as compared with their non-fasting controls during Ramadan fast.97 Based on 36 628 readings by the CGM device and 408 readings by glucose meters the study found that all hypoglycemic episodes occurred between 16:00 and 19:00 hours in both approaches and only 38 readings (9%) of SMBG readings were done in the same time frame indicating that the timing of SMBG missed such hypoglycemic episodes. The rate of hyperglycemia was 5.7% and 14.2% and hypoglycemia was 4.4% and 1.5% using CGM and glucose meters, respectively.
Hyperglycemia in pregnancy is associated with adverse pregnancy outcomes98 and early strict glycemic control during pregnancy is critical to prevent higher risk of hypoglycemia.99 100 Adding the burden of fasting to the complicated state of health in pregnant women with diabetes is not prudent or recommended due to increased risk of hypoglycemia and hyperglycemia.
Fetal outcomes
Studies looking at the effects of fasting on fetal outcomes varied in design and have shown conflicting outcomes. One prospective study in the Netherlands using self-reported data in 130 Muslim pregnant women on adherence to Ramadan fasting during pregnancy reported that 50% of women were adherent to fasting.101 Among them, the birth weight of newborns did not show a statistically significant difference, but it tended to be lower than that of newborns of non-fasting mothers. A meta-analysis pooled data from 22 studies and included 31 374 pregnancies of whom 18 920 were exposed to Ramadan fasting.94 This study’s primary outcome, preterm delivery, was not impacted by fasting during Ramadan and one of the secondary outcomes, birth weight, was not affected by maternal fasting. However, placental weight was significantly lower in fasting mothers, putting in consideration that this observation was dominated by a single large study.102
The possible effect of nutritional restriction and how it can impact the development of the placental enzyme required to convert cortisol to its inactive form may result in a state of prolonged elevation of hypothalamic-pituitary-adrenal axis function which is detrimental and is linked to long-term health consequences such as type 2 diabetes, hypertension and cognitive impairment.103 104
Another study found that the incidence of GDM was significantly higher in the fasting group compared with control group. Furthermore, there was a high rate of induction of labor ~16%, cesarean section as well as higher admissions to the special care baby unit in the fasted group as compared with control group.105
Pregnant women with diabetes or GDM are at high risk of negative maternal and fetal outcome, they should be advised to avoid fasting.
REGIONAL PECULIARITIES OF DIABETES DURING RAMADAN
Egypt
Egypt ranks among the top 10 countries for the number of adult people with diabetes.6 The cultural norm for Egyptian Muslims with diabetes is to fast during Ramadan. Unlike those from the Arab Gulf and North African nations, the majority of Egyptian Muslims break their fast by consuming the main meal (Iftaar) immediately after sunset. In contrast to traditional Muslim teachings of moderation in food intake, this main meal is seen as an opportunity to feast.
Saudi Arabia
Ramadan is a month of nocturnal life in Saudi Arabia. Ramadan fasting in the Kingdom of Saudi Arabia, unlike other Muslim and Arab countries, is associated with profound changes in sleeping and feeding patterns, with an almost complete reversal of the rest/sleep versus wake cycle and restriction of food intake to night-time only.106 Working hours for school and offices are reduced to 6 hours during working days for people to rest before and after Suhoor and Iftaar.
According to a recent study, Saudis fasting during Ramadan stay up at night and sleep through much of the day, mimicking the patterns of shift workers.107 In a cross-sectional study in Riyadh, it was observed that most patients with diabetes (76%) were able to fast during Ramadan.30 Hypoglycemic episodes were reported in 60% in people with type 1 diabetes and in 8% in those with type 2 diabetes. It was concluded that over half of the patients with diabetes who fast during Ramadan may alter their medicines schedule without seeking medical advice.108
Pakistan
A study regarding baseline knowledge of family physicians across the country found that almost one-third of physicians had incorrect perceptions and misbeliefs regarding management of diabetes during Ramadan fasting.109 Another study reported that skin prick for SMBG would make the fast void; as a consequence, 40% of participants who were taking insulin never checked their blood glucose levels during fasting.110
The recommendations given by Ramadan Prospective Diabetes Study Group is to reduce the pre-Suhoor dose of oral glucose-lowering medications or insulin to 75% of the total dose, especially when the drug has to be given within 12 hours.111
The dietary habits with consumption of high carbohydrates, fats and sweets are common in Pakistan.112
Lebanon, Jordan and Palestine
In Lebanon, people with diabetes continue their daily work, but with less physical activity and less sleep. Usually, they consume two large meals between sunset and dawn. Studies in the Middle East where Lebanon took part reported that SMBG and glucose-lowering drugs are safe to be used during Ramadan. In the Lira Ramadan and VIRTUE studies, the liraglutide and vildagliptin groups had a lower rate of hypoglycemic events, better glycemic and weight control compared with the SU groups.60 113 In Canagliflozin in Ramadan Tolerance Observational Study, patients with type 2 diabetes receiving canagliflozin had an increased risk of volume depletion events.55 Among patients treated with insulin, the insulin degludec/aspart group had a lower risk of hypoglycemia than the biphasic insulin aspart 30 group.114 Also, switching from SU to lixisenatide in patients on basal insulin was found to be safe in the LixiRam study.115 GLP-1RAs (liraglutide or dulaglutide), metformin, DPP4 inhibitors (vildagliptin, linagliptin, sitagliptin, alogliptin, saxagliptin), SGLT2i (empagliflozin, dapagliflozin, canagliflozin, ertugliflozin) and TZD (pioglitazone) are usually acceptable treatment options when adjusted to respond to patients’ habits in Ramadan. The incidence of hypoglycemia in the Middle East is higher during Ramadan.116
A prospective, observational, open-label study conducted in Jordan to assess the safety of a protocol involving dose adjustments to four different glucose-lowering drug regimens in patients with type 2 diabetes who chose to fast during Ramadan concluded that no cases were reported of DKA or hyperosmolar state among different regimens and hypoglycemia occurred at a lower rate than pre-Ramadan values, especially in those who were treated with premixed 70/30 insulin, insulin glargine and regular insulin.117 Another in Palestine found that Ramadan fasting is tolerable by hemodialysis patients. However, the potential risk of fluid overload and hyperkalemia must be closely monitored.118
North Africa
In Algeria, patients with both type 1 diabetes and type 2 diabetes fast despite their physicians’ recommendations. Iftaar is usually a very heavy meal that consists of many courses with no breaks in between, unlike people in other Muslim cultures in North Africa who rest in between courses. Once the meal is done, Algerian people spend the evening around coffee, tea and different kinds of pastries. During the evening, men and few women usually go to the mosque for the Taraweeh prayer.119 During Ramadan SMBG is rarely checked.120 As in other Muslim countries, severe hypoglycemia is the main reason for hospitalization in Algeria during the Holy month. Ketoacidosis, dehydration, orthostatic hypotension and thrombosis are some of the other complications that people with diabetes are exposed to during fasting.121 122
In Tunisia, the majority of people with type 1 and type 2 diabetes fast during Ramadan while receiving insulin. In a Tunisian observational study in patients with diabetes treated with insulin during the month of Ramadan, 10% had type 1 diabetes.123 In this study population, 72% reported having fasted without insulin interruption during the month of Ramadan. The average number of non-fasted days was 3 days, mainly due to hypoglycemic episodes. Another study looked at patients with ≥2 cardiovascular risk factors to evaluate metabolic effects of fasting during Ramadan month.124 There was a significant decrease in HbA1c after Ramadan (75 mmol/mol (9.0%) to 60 mmol/mol (7.6%)). No acute metabolic incidents were reported during the study period.
CONCLUSION
Fasting the Holy month of Ramadan constitutes one of the five pillars of the Muslim faith. Illness such as diabetes constitutes an exemption from fasting. Although there is some evidence that intermittent fasting may be of benefit in losing weight and some cardiometabolic benefits, yet, there is little evidence that this may be applicable on people with diabetes.
The ADA/EASD consensus recommendations for diabetes management emphasize the need to consider patient factors including comorbidities when deciding on medication selections. The general principles included in the decision cycle in the ADA/EASD consensus applies to Ramadan taking into consideration the presence of comorbidities like ASCVD, HF and CKD, risk of hypoglycemia, weight issues and cost-effectiveness. Care should be individualized with shared decision making between the provider and the patient. Structured education and pre-Ramadan counseling are key components to successful management of diabetes for patients during Ramadan. These should cover all important aspects like glycemic targets during Ramadan, SMBG, diet, physical activity including Taraweeh prayers, glucose-lowering medication dose adjustments and side effects and decision when to break the fast. The decision cycle in figure 1 adapted for the specific situation of Ramadan provides an aid for such an assessment.
People with type 2 diabetes and multiple serious comorbidities and diabetic complications, as well as patients with type 1 diabetes should strongly be advised not to fast considering the very high risk of developing complications. Pregnant women with diabetes or GDM should also be advised to skip fasting because of the possible negative maternal and fetal outcomes.
The use of the emerging technologies and CGM during Ramadan could optimize the outcome, although the cost is a significant barrier. Ongoing support and monitoring remain integral to a successful outcome and a proper management plan is required. Ramadan guidance for patients with diabetes should be reviewed periodically in the light of new emerging evidence and technology.
References
Footnotes
Contributors MI determined the manuscript strategy, wrote the first draft, he also wrote a section about Egypt and fixed the coauthors’ comments on each version; MJD, EA and KK wrote a section about the ADA/EASD consensus and the related figures; FAA wrote a section about Jordan; RHE wrote a section about children with type 1 diabetes; EMB-E wrote sections about intermittent fasting and also section about Saudi Arabia along with dates consumption; NAES wrote a section about pregnancy; AHF wrote a section about nutrition and hypoglycemia; PH wrote a section about Lebanon; HI, IK and SM-Z wrote a section about north Africa; SNM and SS wrote a section about Pakistan; JT and GEU provided intellectual content in interpreting data and critically reviewed the manuscript. All authors revised and approved the final version of the manuscript.
Funding This research was supported by the National Institute for Health Research (NIHR) Leicester Biomedical Research Centre (BRC), the NIHR Leicester Clinical Research Facility (CRF) and the NIHR Applied Research Collaboration East Midlands (ARC–EM).
Disclaimer The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health and Social Care.
Competing interests None declared.
Patient consent for publication Not required.
Provenance and peer review Not commissioned; externally peer reviewed.
Data availability statement All data relevant to the study are included in the article. De-identified participant data.