Abstract
Purpose
Diabetic patients tend to have a poor quality of life. A sedentary lifestyle is considered to be a modifiable risk factor for type 2 diabetes and an independent predictor of poor quality of life. Exercise is a key treatment for people living with diabetes. The purpose of this study was to conduct a systematic review to assess the effect of exercise on the quality of life of people with type 2 diabetes.
Methods
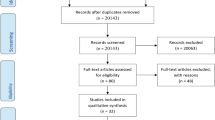
We conducted a systematic review using the Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines. PubMed, Web of Science, Embase, Cochrane Library, CINAHL and three Chinese databases were searched for studies published until January 2016. The review included all clinical trials that evaluated the effect of exercise on quality of life compared with that of usual care for people with type 2 diabetes. Two reviewers independently assessed the quality of all the included studies, by using the Downs and Black Quality Index (QI).
Results
Thirty studies met inclusion criteria, with 2785 participants. We divided the exercise into four modes: aerobic, resistance, a combination of aerobic and resistance and yoga. Aerobic exercise showed a significant effect between groups. Resistance and combined exercise showed mixed results. Yoga also showed good intervention effects on quality of life.
Conclusions
The effect of aerobic exercise on the quality of life in people with type 2 diabetes was safe and effective. Then, most of the studies on aerobic exercise were of good methodological quality. The effects of resistance exercise and combined exercise on the quality of life in people with type 2 diabetes were mixed, and the effect of yoga on quality of life still need more research.

Similar content being viewed by others
Abbreviations
- VAS:
-
Visual Analogue Scale
- CES-D:
-
Center for Epidemiologic Depression Scale
- EuroQoL:
-
European Quality of Life Questionnaire
- SF-12:
-
12-item Short-Form Health Survey
- SF-36:
-
36-item Short-Form Health Survey
- WHOQol-BREF:
-
World Health Organization Quality of Life questionnaire
- PCS:
-
Physical Component Summary
- SWED-QUAL:
-
Swedish Health-Related Quality of Life questionnaire
- QOLOD:
-
Quality of Life, Obesity and Dietetics questionnaire
- NQOL:
-
Neuropathy-specific Quality of Life instrument
- ADS-L:
-
German version of the general depression scale CES-D, ADS-L (Allgemeine Depressionsskala)
- DCCT:
-
Diabetes Control and Complication Trial
- HbA1c :
-
Haemoglobin A1c
- BMI:
-
Body mass index
- T2DM:
-
Type 2 diabetes mellitus
- NYHA:
-
New York Heart Association
- RCT:
-
Randomized control trials
- PCS:
-
Physical component score
- MCS:
-
Mental component score
- ES:
-
Effect size
References
Shaw, J. E., Sicree, R. A., & Zimmet, P. Z. Global estimates of the prevalence of diabetes for 2010 and 2030. Diabetes Research and Clinical Practice, 87(1), 4–14. doi:10.1016/j.diabres.2009.10.007.
Godman, B., Malmstrom, R. E., Diogene, E., Gray, A., Jayathissa, S., Timoney, A., et al. (2014). Are new models needed to optimize the utilization of new medicines to sustain healthcare systems? Expert Review of Clinical Pharmacology, 8(1), 77–94. doi:10.1586/17512433.2015.990380.
Gregg, E. B. G., Williamson, D., Lev-eille, S., Langlois, J., Engelgau, M., & Narayan, K. M. (2000). Diabetes and physical disabilityamong older U.S. adults. Diabetes Care, 23, 1272–1277.
Glasgow, R. E., Ruggiero, L., Eakin, E. G., Dryfoos, J., & Chobanian, L. (1997). Quality of life and associated characteristics in a large national sample of adults with diabetes. Diabetes Care, 20(4), 562–567.
Al-Aboudi, I. S., Hassali, M. A., Shafie, A. A., Hassan, A., & Alrasheedy, A. A. (2015). A cross-sectional assessment of health-related quality of life among type 2 diabetes patients in Riyadh, Saudi Arabia. SAGE Open Medicine, 3, 2050312115610129. doi:10.1177/2050312115610129.
Healy, G. N., Wijndaele, K., Dunstan, D. W., Shaw, J. E., Salmon, J., Zimmet, P. Z., et al. (2008). Objectively measured sedentary time, physical activity, and metabolic risk: The Australian diabetes, obesity and lifestyle study (AusDiab). Diabetes Care, 31(2), 369–371. doi:10.2337/dc07-1795.
Wilmot, E. G., Edwardson, C. L., Achana, F. A., Davies, M. J., Gorely, T., Gray, L. J., et al. (2012). Sedentary time in adults and the association with diabetes, cardiovascular disease and death: Systematic review and meta-analysis. Diabetologia, 55(11), 2895–2905. doi:10.1007/s00125-012-2677-z.
Grontved, A., & Hu, F. B. (2011). Television viewing and risk of type 2 diabetes, cardiovascular disease, and all-cause mortality: A meta-analysis. JAMA, 305(23), 2448–2455. doi:10.1001/jama.2011.812.
Cooper, A. R., Sebire, S., Montgomery, A. A., Peters, T. J., Sharp, D. J., Jackson, N., et al. (2011). Sedentary time, breaks in sedentary time and metabolic variables in people with newly diagnosed type 2 diabetes. Diabetologia, 55(3), 589–599. doi:10.1007/s00125-011-2408-x.
Grp, U. P. D. S. (1999). Tight blood pressure control and risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 38 (vol 317, pg 703, 1998). Bmj-British Medical Journal, 318(7175), 29.
Wandell, P. E. (2005). Quality of life of patients with diabetes mellitus—an overview of research in primary health care in the Nordic countries. Scandinavian Journal of Primary Health Care, 23(2), 68–74. doi:10.1080/02813430510015296.
Landman, G. W., van Hateren, K. J., Kleefstra, N., Groenier, K. H., Gans, R. O., & Bilo, H. J. (2010). Health-related quality of life and mortality in a general and elderly population of patients with type 2 diabetes (ZODIAC-18). Diabetes Care, 33(11), 2378–2382. doi:10.2337/dc10-0979.
Huang, E. S., Brown, S. E., Ewigman, B. G., Foley, E. C., & Meltzer, D. O. (2007). Patient perceptions of quality of life with diabetes-related complications and treatments. Diabetes Care, 30(10), 2478–2483. doi:10.2337/dc07-0499.
Sudeck, G., & Honer, O. (2011). Volitional Interventions within cardiac exercise therapy (VIN-CET): Long-term effects on physical activity and health-related Quality of life. Applied Psychology-Health and Well Being, 3(2), 151–171. doi:10.1111/j.1758-0854.2010.01047.x.
Umpierre, D., Ribeiro, P. A., Kramer, C. K., Leitao, C. B., Zucatti, A. T., Azevedo, M. J., et al. (2011). Physical activity advice only or structured exercise training and association with HbA1c levels in type 2 diabetes: A systematic review and meta-analysis. JAMA, 305(17), 1790–1799. doi:10.1001/jama.2011.576.
Boule, N. G., Haddad, E., Kenny, G. P., Wells, G. A., & Sigal, R. J. (2001). Effects of exercise on glycemic control and body mass in type 2 diabetes mellitus: A meta-analysis of controlled clinical trials. JAMA, 286(10), 1218–1227.
Conn, V. S., Hafdahl, A. R., Mehr, D. R., LeMaster, J. W., Brown, S. A., & Nielsen, P. J. (2007). Metabolic effects of interventions to increase exercise in adults with type 2 diabetes. Diabetologia, 50(5), 913–921. doi:10.1007/s00125-007-0625-0.
Snowling, N. J., & Hopkins, W. G. (2006). Effects of different modes of exercise training on glucose control and risk factors for complications in type 2 diabetic patients: A meta-analysis. Diabetes Care, 29(11), 2518–2527. doi:10.2337/dc06-1317.
Dunstan, D. W., Kingwell, B. A., Larsen, R., Healy, G. N., Cerin, E., Hamilton, M. T., et al. (2012). Breaking up prolonged sitting reduces postprandial glucose and insulin responses. Diabetes Care, 35(5), 976–983. doi:10.2337/dc11-1931.
Duvivier, B. M. F. M., Schaper, N. C., Bremers, M. A., van Crombrugge, G., & Menheere, P. P. C. A. (2014). Minimal intensity physical activity (standing and walking) of longer duration improves insulin action and plasma lipids more than shorter periods of moderate to vigorous exercise (cycling) in sedentary subjects when energy expenditure is comparable (vol 8, e55542, 2013). PLoS One. doi:10.1371/journal.pone.0105135.
Green, A. J., Fox, K. M., & Grandy, S. (2011). Impact of regular exercise and attempted weight loss on quality of life among adults with and without type 2 diabetes mellitus. Journal of Obesity. doi:10.1155/2011/172073.
Imayama, I., Plotnikoff, R. C., Courneya, K. S., & Johnson, J. A. (2010). Determinants of quality of life in type 2 diabetes population: the inclusion of personality. Quality of Life Research, 20(4), 551–558. doi:10.1007/s11136-010-9772-8.
Caspersen, C. J., Powell, K. E., & Christenson, G. M. (1985). Physical activity, exercise, and physical fitness: definitions and distinctions for health-related research. Public Health Reports, 100(2), 126–131.
Youngstedt, S. D., O’Connor, P. J., & Dishman, R. K. (1997). The effects of acute exercise on sleep: A quantitative synthesis. Sleep, 20(3), 203–214.
Breneman, C. B., Porter, R. R., Iftikhar, I., Smith, S., & Wang, X. W. (2014). The relationship between aerobic fitness and physical activity with sleep characteristics in sedentary older women. Medicine and Science in Sports and Exercise, 46(5), 654–655.
Talbot, L. S., Neylan, T. C., Metzler, T. J., & Cohen, B. E. (2014). The mediating effect of sleep quality on the relationship between PTSD and physical activity. Journal of Clinical Sleep Medicine, 10(7), 795–801. doi:10.5664/jcsm.3878.
Hillsdon, M. M., Brunner, E. J., Guralnik, J. M., & Marmot, M. G. (2005). Prospective study of physical activity and physical function in early old age. American Journal of Preventive Medicine, 28(3), 245–250. doi:10.1016/j.amepre.2004.12.008.
van der Heijden, M. M. P., van Dooren, F. E. P., Pop, V. J. M., & Pouwer, F. (2013). Effects of exercise training on quality of life, symptoms of depression, symptoms of anxiety and emotional well-being in type 2 diabetes mellitus: A systematic review. Diabetologia, 56(6), 1210–1225. doi:10.1007/s00125-013-2871-7.
Moher, D., Liberati, A., Tetzlaff, J., & Altman, D. G. (2009). Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Journal of Clinical Epidemiology, 62(10), 1006–1012. doi:10.1016/j.jclinepi.2009.06.005.
Downs, S. H., & Black, N. (1998). The feasibility of creating a checklist for the assessment of the methodological quality both of randomised and non-randomised studies of health care interventions. Journal of Epidemiology and Community Health, 52(6), 377–384.
Higgins, T., & Julian, P. (2008). Cochrane handbook for systematic reviews of interventions. Wiley.
Ahn, S., & Song, R. (2012). Effects of Tai Chi Exercise on glucose control, neuropathy scores, balance, and quality of life in patients with type 2 diabetes and neuropathy. Journal of Alternative and Complementary Medicine, 18(12), 1172–1178. doi:10.1089/acm.2011.0690.
Asa, C., Maria, S., Katharina, S. S., & Bert, A. (2012). Aquatic exercise is effective in improving exercise performance in patients with heart failure and type 2 diabetes mellitus. Evidence-Based Complementary and Alternative Medicine, 2012, 8. doi:10.1155/2012/349209.
Aylin, K., Arzu, D., Sabri, S., Handan, T. E., & Ridvan, A. (2009). The effect of combined resistance and home-based walking exercise in type 2 diabetes patients. International Journal of Diabetes in Developing Countries, 29(4), 159–165. doi:10.4103/0973-3930.57347.
Baillot, A., Vibarel-Rebot, N., Amiot, V., Emy, P., & Collomp, K. (2012). Effects of an 8-week aerobic exercise training on saliva steroid hormones, physical capacity, and quality of life in diabetic obese men. Hormone and Metabolic Research, 44(2), 146–151. doi:10.1055/s-0031-1297262.
Bennett, W. L., Ouyang, P., Wu, A. W., Barone, B. B., & Stewart, K. J. (2008). Fatness and fitness: How do they influence health-related quality of life in type 2 diabetes mellitus? Health and Quality of Life Outcomes. doi:10.1186/1477-7525-6-110.
Bello, A. I., Owusu-Boakye, E., Adegoke, B. O., & Adjei, D. N. (2011). Effects of aerobic exercise on selected physiological parameters and quality of life in patients with type 2 diabetes mellitus. Int J Gen Med, 4, 723–727. doi:10.2147/IJGM.S16717.
Cheung, N. W., Cinnadaio, N., Russo, M., & Marek, S. (2009). A pilot randomised controlled trial of resistance exercise bands in the management of sedentary subjects with type 2 diabetes. Diabetes Research and Clinical Practice, 83(3), e68–e71. doi:10.1016/j.diabres.2008.12.009.
Cugusi, L., Cadeddu, C., Nocco, S., Orru, F., Bandino, S., Deidda, M., et al. (2015). Effects of an aquatic-based exercise program to improve cardiometabolic profile, quality of life, and physical activity levels in men with type 2 diabetes mellitus. Pm&R, 7(2), 141–148. doi:10.1016/j.pmrj.2014.09.004.
Dede, N. D., Ipekci, S. H., Kebapcilar, L., Arslan, M., Kurban, S., Yildiz, M., et al. (2015). Influence of exercise on leptin, adiponectin and quality of life in type 2 diabetics. Turkish Journal of Endocrinology and Metabolism, 19(1), 7–13. doi:10.4274/tjem.2564.
Dixit, S., Maiya, A., & Shastry, B. (2014). Effect of aerobic exercise on quality of life in population with diabetic peripheral neuropathy in type 2 diabetes: A single blind, randomized controlled trial. Quality of Life Research, 23(5), 1629–1640. doi:10.1007/s11136-013-0602-7.
Eckert, K. (2012). Impact of physical activity and bodyweight on health-related quality of life in people with type 2 diabetes. Diabetes Metab Syndr Obes, 5, 303–311. doi:10.2147/DMSO.S34835.
Ferrer-Garcia, J. C., Sanchez Lopez, P., Pablos-Abella, C., Albalat-Galera, R., Elvira-Macagno, L., Sanchez-Juan, C., et al. (2011). Benefits of a home-based physical exercise program in elderly subjects with type 2 diabetes mellitus. Endocrinología y Nutrición, 58(8), 387–394. doi:10.1016/j.endonu.2011.05.010.
Fritz, T., Caidahl, K., Osler, M., Ostenson, C. G., Zierath, J. R., & Wandell, P. (2011). Effects of Nordic walking on health-related quality of life in overweight individuals with type 2 diabetes mellitus, impaired or normal glucose tolerance. Diabetic Medicine, 28(11), 1362–1372. doi:10.1111/j.1464-5491.2011.03348.x.
Gram, B., Christensen, R., Christiansen, C., & Gram, J. (2010). Effects of Nordic walking and exercise in type 2 diabetes mellitus: A randomized controlled trial. Clinical Journal of Sport Medicine, 20(5), 355–361. doi:10.1227/NEU.0b013e3181e56e0a.
Holton, D. R., Colberg, S. R., Nunnold, T., Parson, H. K., & Vinik, A. I. (2003). The effect of an aerobic exercise training program on quality of life in type 2 diabetes. The Diabetes Educator, 29(5), 837–846.
Kempf, K., & Martin, S. (2013). Autonomous exercise game use improves metabolic control and quality of life in type 2 diabetes patients—a randomized controlled trial. Bmc Endocrine Disorders. doi:10.1186/1472-6823-13-57.
Krousel-Wood, M. A., Berger, L., Jiang, X., Blonde, L., Myets, L., & Webber, L. (2008). Does home-based exercise improve body mass index in patients with type 2 diabetes? Results of a feasibility trial. Diabetes Research and Clinical Practice, 79(2), 230–236. doi:10.1016/j.diabres.2007.08.028.
Labrunee, M., Antoine, D., Verges, B., Robin, I., Casillas, J. M., & Gremeaux, V. (2012). Effects of a home-based rehabilitation program in obese type 2 diabetics. Annals of Physical and Rehabilitation Medicine, 55(6), 415–429. doi:10.1016/j.rehab.2012.06.001.
Lambers, S., Van Laethem, C., Van Acker, K., & Calders, P. (2008). Influence of combined exercise training on indices of obesity, diabetes and cardiovascular risk in type 2 diabetes patients. Clinical Rehabilitation, 22(6), 483–492. doi:10.1177/0269215508084582.
Lincoln, A. K., Shepherd, A., Johnson, P. L., & Castaneda-Sceppa, C. (2011). The impact of resistance exercise training on the mental health of older Puerto Rican adults with type 2 diabetes. Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 66(5), 567–570. doi:10.1093/geronb/gbr034.
Liu, X., Miller, Y. D., Burton, N. W., Chang, J. H., & Brown, W. J. (2013). The effect of Tai Chi on health-related quality of life in people with elevated blood glucose or diabetes: a randomized controlled trial. Quality of Life Research, 22(7), 1783–1786. doi:10.1007/s11136-012-0311-7.
Myers, V. H., McVay, M. A., Brashear, M. M., Johannsen, N. M., Swift, D. L., Kramer, K., et al. (2013). Exercise training and quality of life in individuals with type 2 diabetes: A randomized controlled trial. Diabetes Care, 36(7), 1884–1890. doi:10.2337/dc12-1153.
Nicolucci, A., Balducci, S., Cardelli, P., Cavallo, S., Fallucca, S., Bazuro, A., et al. (2012). Relationship of exercise volume to improvements of quality of life with supervised exercise training in patients with type 2 diabetes in a randomised controlled trial: The Italian diabetes and exercise study (IDES). Diabetologia, 55(3), 579–588. doi:10.1007/s00125-011-2425-9.
Plotnikoff, R. C., Eves, N., Jung, M., Sigal, R. J., Padwal, R., & Karunamuni, N. (2010). Multicomponent, home-based resistance training for obese adults with type 2 diabetes: A randomized controlled trial. International Journal of Obesity (London), 34(12), 1733–1741. doi:10.1038/ijo.2010.109.
Reid, R. D., Tulloch, H. E., Sigal, R. J., Kenny, G. P., Fortier, M., McDonnell, L., et al. (2010). Effects of aerobic exercise, resistance exercise or both, on patient-reported health status and well-being in type 2 diabetes mellitus: A randomised trial. Diabetologia, 53(4), 632–640. doi:10.1007/s00125-009-1631-1.
Sazlina, S. G., Browning, C. J., & Yasin, S. (2015). Effectiveness of personalized feedback alone or combined with peer support to improve physical activity in sedentary older malays with type 2 diabetes: A randomized controlled trial. Front Public Health, 3, 178. doi:10.3389/fpubh.2015.00178.
Tessier, D., Menard, J., Fulop, T., Ardilouze, J., Roy, M., Dubuc, N., et al. (2000). Effects of aerobic physical exercise in the elderly with type 2 diabetes mellitus. Archives of Gerontology and Geriatrics, 31(2), 121–132.
Tsang, T., Orr, R., Lam, P., Comino, E. J., & Singh, M. F. (2007). Health benefits of Tai Chi for older patients with type 2 diabetes: The “Move It for Diabetes Study”—a randomized controlled trial. Clinical Interventions in Aging, 2(3), 429–439.
Viveka, P. J., Joshi, A., Ambekar, S., Kumar, N., Dhawan, A., & Sreenivas, V. (2012). Comprehensive yogic breathing improves quality of life in diabetes. Indian Journal of Endocrinology and Metabolism, 16(3), 5.
Kirk, A. F., Higgins, L. A., Hughes, A. R., Fisher, B. M., Mutrie, N., Hillis, S., et al. (2001). A randomized, controlled trial to study the effect of exercise consultation on the promotion of physical activity in people with type 2 diabetes: A pilot study. Diabetic Medicine, 18(11), 877–882.
Balducci, S., Zanuso, S., Massarini, M., Corigliano, G., Nicolucci, A., Missori, S., et al. (2008). The Italian diabetes and exercise study (ides): Design and methods for a prospective italian multicentre trial of intensive lifestyle intervention in people with type 2 diabetes and the metabolic syndrome. Nutrition, Metabolism and Cardiovascular Diseases, 18(9), 585–595. doi:10.1016/j.numecd.2007.07.006.
Korkiakangas, E., Taanila, A. M., & Keinanen-Kiukaanniemi, S. (2011). Motivation to physical activity among adults with high risk of type 2 diabetes who participated in the Oulu substudy of the finnish diabetes prevention study. Health and Social Care in the Community, 19(1), 15–22. doi:10.1111/j.1365-2524.2010.00942.x.
From the Centers for Disease Control and Prevention. (1993). Public health focus: Physical activity and the prevention of coronary heart disease. JAMA, 270(13), 1529–1530.
Funding
Work on this manuscript was supported by Youth Program of Health and Family Planning Commission of Jilin Province (2015Q022).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Hong Cai and Guichen Li have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Cai, H., Li, G., Zhang, P. et al. Effect of exercise on the quality of life in type 2 diabetes mellitus: a systematic review. Qual Life Res 26, 515–530 (2017). https://doi.org/10.1007/s11136-016-1481-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-016-1481-5